Bone marrow transplantation is an effective method of treating diseases of the blood system, congenital and acquired immunodeficiencies. It is also used to treat autoimmune diseases of the nervous system and connective tissue, and certain forms of malignant neoplasms in children and adults (Figure 1). More than 50,000 bone marrow transplants are performed worldwide each year Aljurf, et al., 2019). For many patients, transplantation has given them a chance to get rid of terrible diseases (Kliman et al., 2020). Transplantation allows long and stable remission of the disease when traditional treatment is powerless.

History of the Origins of Bone Marrow Transplantation
Already by the beginning of the 1950s, scientists had realized that blood cells could develop from some few cells in the bone marrow; such bone marrow cells began to be called stem cells. Later, the idea emerged that stem cells from the bone marrow of a healthy person could be used to restore another person’s bone marrow that was not working. In other words, cells from one person’s bone marrow could be transplanted to another person for therapeutic purposes. Nevertheless, the history of the emergence and development of allogeneic bone marrow transplantation is actually short. Only several decades have passed since the world’s first successful surgery of this type. However, an enormous amount of work has been done in this small period (Figure 1). The results of animal bone marrow transplantation studies have stimulated interest among researchers to conduct similar experiments in humans (Khaddour et al., 2021). Nevertheless, certainly, there was no evidence that the treatment performed on animals could be applied in humans.

The first publication on the use of such surgery appeared in 1957 (Simpson & Dazzi, 2019). As early as 1977, the results of the treatment of the first 100 patients were published (Gorin, 2021). Since the end of the 1970s, there has been an intensive improvement in cellular therapy (Gorin, 2021). In the mid-80s, the results of transplants performed on patients in remission of leukemia appeared – they were encouraging. Since that time, this treatment method began to spread rapidly in hematology, the number of transplants increased from year to year. By 1990, more than 4,000 allogeneic bone marrow transplants had been performed worldwide (Thomas, 2018). Every year the popularity of this type of treatment continues to grow at an intense rate.
Clinical Use of Bone Marrow Transplantation
Bone marrow transplants involve injecting healthy hematopoietic cells into the human body to replace damaged or diseased cells. More often than not, stem cells are taken from blood, not bone marrow. Therefore, the procedure is often called a blood stem cell transplant. The surgery is used as a potential cure for some dangerous oncohematological diseases and non-malignant blood diseases (D’Souza et al., 2017). Bone marrow transplants are necessary when blood fails to perform its functions (D’Souza et al., 2017). This procedure is effective for a variety of diseases, including severe forms of aplastic anemia, tumor diseases of the blood, and severe damage to the immune system.
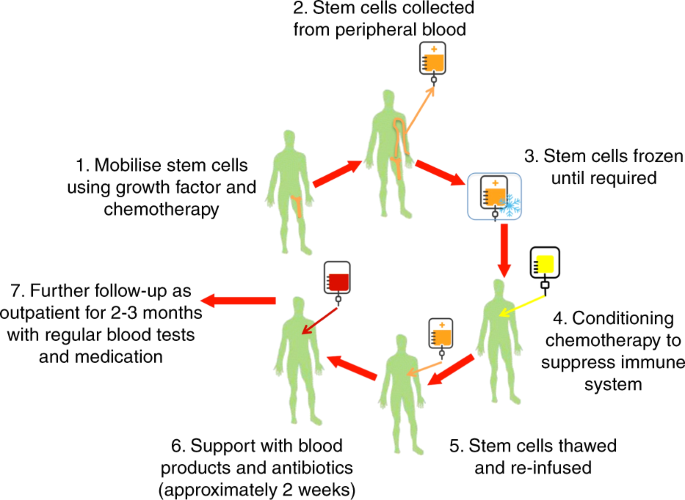
Depending on the source of transplanted cells, allogeneic stem cell transplant, autologous stem cell transplant, and syngeneic stem cell transplant are distinguished. The principle of the operation is illustrated in detail in the diagram below (Figure 1). In the first type of transplantation, the source of hematopoietic cells is a healthy person who has a genetic similarity with the patient according to certain genetic parameters. In autologous stem cell transplantation, the stem cells or bone marrow source is the patient himself. In syngeneic transplantation, the donor is the patient’s monozygotic, in other words, genetically similar twin.

The hematopoietic cells contained in the bone marrow, hematopoietic stem cells of the peripheral blood, hematopoietic cells of the umbilical cord blood are used for the alogical transformation. The probability of a genetic match of the similarity of the hematopoietic tissue of relatives is no more than 25%. (Clancy et al., 2019). Therefore, recently, partially matched hematopoietic cells from unrelated donors are increasingly being used. The search for an unrelated donor is performed in the bone marrow donor registry, in which a donor compatible with the patient is selected. Compatibility is determined after laboratory tests that determine the genetic profile of the donor and patient tissues; this study is called HLA typing.
Since the mid-1970s, bone marrow has been used less frequently for transplantation due to the emergence of special equipment for obtaining stem cells from peripheral blood. Blood cell separators have made the procedure of obtaining hematopoietic stem cells much more efficient and safe. The obtained product of hematopoietic stem cells is frozen and stored for the required time in a liquid nitrogen at -197°C (Berz et al., 2007). The thawed cells are then returned to the patient by intravenous infusion. As a rule, intensive chemotherapy is given before transplantation to remove the tumor cells from the body. This process also allows them to overcome their drug resistance to chemotherapy.
Algorithm of the Operation
After deciding on the advisability of a bone marrow transplant, the algorithm for action consists of several steps. First, there is a thorough diagnosis to rule out the presence of infections in the body. Next, the doctor takes and prepares the graft (donor or autologous); the method of biomaterial processing depends on the diagnosis and several other factors. The patient then undergoes high-dose chemotherapy to kill the abnormal bone marrow cells, followed by bone marrow transplant surgery (Figure 2). Isolation and postoperative monitoring are provided to avoid infections and other postoperative complications (Simpson & Dazzi, 2019). At the end of the procedure, patients are transferred to a special room with a laminar flow, where they remain until the bone marrow engrafts. Outpatient observation is also mandatory, with regular blood tests and other necessary tests to assess graft engraftment and monitor the underlying disease.
Doctors evaluate the results of various blood tests to confirm the production of new blood cells and the absence of recurrence. After transplantation, patients have blood drawn daily for laboratory analysis (Sharma et al., 2021). White blood cells are the first to engraft, followed by red blood cells and platelets. Patients may need transfusions of red blood cells and platelets to maintain an adequate supply during grafting (Hosoba et al., 2018). Extraction of a small bone marrow sample with a needle for examination under a microscope also allows physicians to assess hematopoietic cell function and the achievement of remission.
Concerns of Patients and Experts
Many patients think that transplantation is a complicated surgical procedure. However, transplantation itself is a relatively simple process similar to a blood transfusion. The donor cells are in a bag or syringe connected through a tube to the patient’s central catheter. The procedure lasts from a few minutes to a few hours and does not cause any pain. After entering the bloodstream, the hematopoietic cells reach the bone marrow, dividing and turning into white blood cells, red blood cells, and platelets. This process is called engraftment and lasts about 2-4 weeks. Full recovery of the immune system can take from several months in autologous transplantation to 6 months or a year in allogeneic transplantation.
Nevertheless, the transplant procedure is a physically demanding ordeal for the patient. Many scientists believe that this procedure can cause many complications for the human body (Figure 1). Doctors should first determine if the patient is a suitable candidate. For this purpose, factors such as age, general physical condition, diagnosis, previous treatment, and availability of the donor are considered. The patient’s heart, lungs, kidneys, and other vital organs are also examined to ensure the transplant will engraft (Michigan Medicine, 2019). The following tests are usually scheduled: examinations to determine current disease status, physical examination, and oral examination. It is also important to have an ECG scan to evaluate heart function and a pulmonary function study.

Many experts are convinced that this treatment method should be used with caution because transplantation is not easy to endure. It involves physical and emotional difficulties for both the patient and family. However, the transplant treatment team includes many people willing to support those going through the process. Meetings are usually scheduled with a financial counselor to discuss insurance and financial issues (Cleveland Clinic, 2019). In addition, the patient’s family is expected to meet with a social worker or psychologist to discuss emotional their well-being. Many children and adolescents who have had transplants are now living full lives and no longer have cancer.
Conclusion
To increase the number of transplants, it is necessary to spread the method more widely, to open new transplantation departments. It is also important to train specialists and increase the number of transplant quotas. Such high-tech methods of medical care as bone marrow transplantation is an example of a multidisciplinary approach in medicine. It is possible only in close cooperation of clinical services with laboratory, functional diagnostics departments, blood transfusion stations, ambulatory care, and bone marrow donor registries. Successes in bone marrow transplantation are crucial medical achievements and contribute to developing and improving medical care.
References
Akbulut, G. (2013). Medical nutritional therapy in hematopoietic stem cell transplantation (HSCT). International Journal of Hematology and Oncology, 23. 55-65. Web.
Aljurf, M., Weisdorf, D., Alfraih, F., Szer, J., Müller, C., Confer, D., Hashmi, S., Kröger, N., Shaw, B. E., Greinix, H., Kharfan-Dabaja, M. A., Foeken, L., Seber, A., Ahmed, S., El-Jawahri, A., Al-Awwami, M., Atsuta, Y., Pasquini, M., Hanbali, A., Alzahrani, H., … El Fakih, R. (2019). Worldwide network for blood & marrow transplantation (WBMT) special article, challenges facing emerging alternate donor registries. Bone Marrow Transplantation, 54(8), 1179–1188. Web.
Berz, D., McCormack, E. M., Winer, E. S., Colvin, G. A., & Quesenberry, P. J. (2007). Cryopreservation of hematopoietic stem cells. American Journal of Hematology, 82(6), 463–472. Web.
Clancy, J., Ritari, J., Lobier, M., Niittyvuopio, R., Salmenniemi, U., Putkonen, M., Itälä-Remes, M., Partanen, J., & Koskela, S. (2019). Increased MHC matching by C4 gene compatibility in unrelated donor hematopoietic stem cell transplantation. Biology of Blood and Marrow Transplantation: Journal of the American Society for Blood and Marrow Transplantation, 25(5), 891–898. Web.
Cleveland Clinic. (2019). Bone marrow transplant: Financial questions to ask. Web.
D’Souza, A., Lee, S., Zhu, X., & Pasquini, M. (2017). Current use and trends in hematopoietic cell transplantation in the United States. Biology of Blood and Marrow Transplantation: Journal of the American Society for Blood and Marrow Transplantation, 23(9), 1417–1421. Web.
Gorin N. C. (2021). History and development of autologous stem cell transplantation for acute myeloid leukemia. Clinical Hematology International, 3(3), 83–95. Web.
Hosoba, S., Waller, E. K., Shenvi, N., Graiser, M., Easley, K. A., Al-Kadhimi, Z., Andoh, A., Antun, A. G., Barclay, S., Josephson, C. D., Koff, J. L., Khoury, H. J., Langston, A. A., Zimring, J. C., Roback, J. D., & Giver, C. R. (2018). Peritransplantation red blood cell transfusion is associated with increased risk of graft-versus-host disease after allogeneic hematopoietic stem cell transplantation. Biology of Blood and Marrow Transplantation: Journal of the American Society for Blood and Marrow Transplantation, 24(5), 973–982. Web.
Inamoto, Y., & Lee, S. J. (2017). Late effects of blood and marrow transplantation. Haematologica, 102(4), 614–625. Web.
Jessop, H., Farge, D., Saccardi, R., Alexander, T., Rovira, M., Sharrack, B., Greco, R., Wulffraat, N., Moore, J., Kazmi, M., Badoglio, M., Adams, G., Verhoeven, B., Murray, J., & Snowden, J. A. (2019). General information for patients and carers considering haematopoietic stem cell transplantation (HSCT) for severe autoimmune diseases (ADs): A position statement from the EBMT Autoimmune Diseases Working Party (ADWP), the EBMT Nurses Group, the EBMT Patient, Family and Donor Committee and the Joint Accreditation Committee of ISCT and EBMT (JACIE). Bone Marrow Transplantation, 54(7), 933–942. Web.
Khaddour, K., Hana, C. K., & Mewawalla, P. (2021). Hematopoietic stem cell transplantation. StatPearls Publishing.
Kliman, D., Nivison-Smith, I., Gottlieb, D., Hamad, N., Kerridge, I., Purtill, D., Szer, J., & Ma, D. (2020). Hematopoietic stem cell transplant recipients surviving at least 2 years from transplant have survival rates approaching population levels in the modern era of transplantation. Biology of Blood and Marrow Transplantation: Journal of the American Society for Blood and Marrow Transplantation, 26(9), 1711–1718. Web.
Michigan Medicine. (2019). Common pre-transplant tests and procedures. Web.
Sharma, A., Badawy, S. M., Suelzer, E. M., Murthy, H. S., Prasad, P., Eissa, H., Carpenter, P. A., Hamadani, M., Labopin, M., Schoemans, H., Tichelli, A., Phelan, R., Hamilton, B. K., Buchbinder, D., Im, A., Hunter, R., Brazauskas, R., & Burns, L. J. (2021). Systematic reviews in hematopoietic cell transplantation and cellular therapy: considerations and guidance from the American Society for Transplantation and Cellular Therapy, European Society for Blood and Marrow Transplantation, and the Center for International Blood and Marrow Transplant Research late effects and quality of life working committee. Bone Marrow Transplantation, 56(4), 786–797. Web.
Simpson, E., & Dazzi, F. (2019). Bone marrow transplantation 1957-2019. Frontiers in Immunology, 10, 1-6. Web.
Stem Med. (2019). A quick look at the history of stem cell research & therapies. Web.
Thomas, E. D. (1990). Bone marrow transpantion – past, present and future. The Fred Hutchinson Cancer Research Center and the University of Washington. Web.
Wynn, R., Bhat, R., & Monagle, P. (2017). Principles of blood and bone marrow transplantation (BMT) in pediatric medicine. Cambridge University Press. Web.